
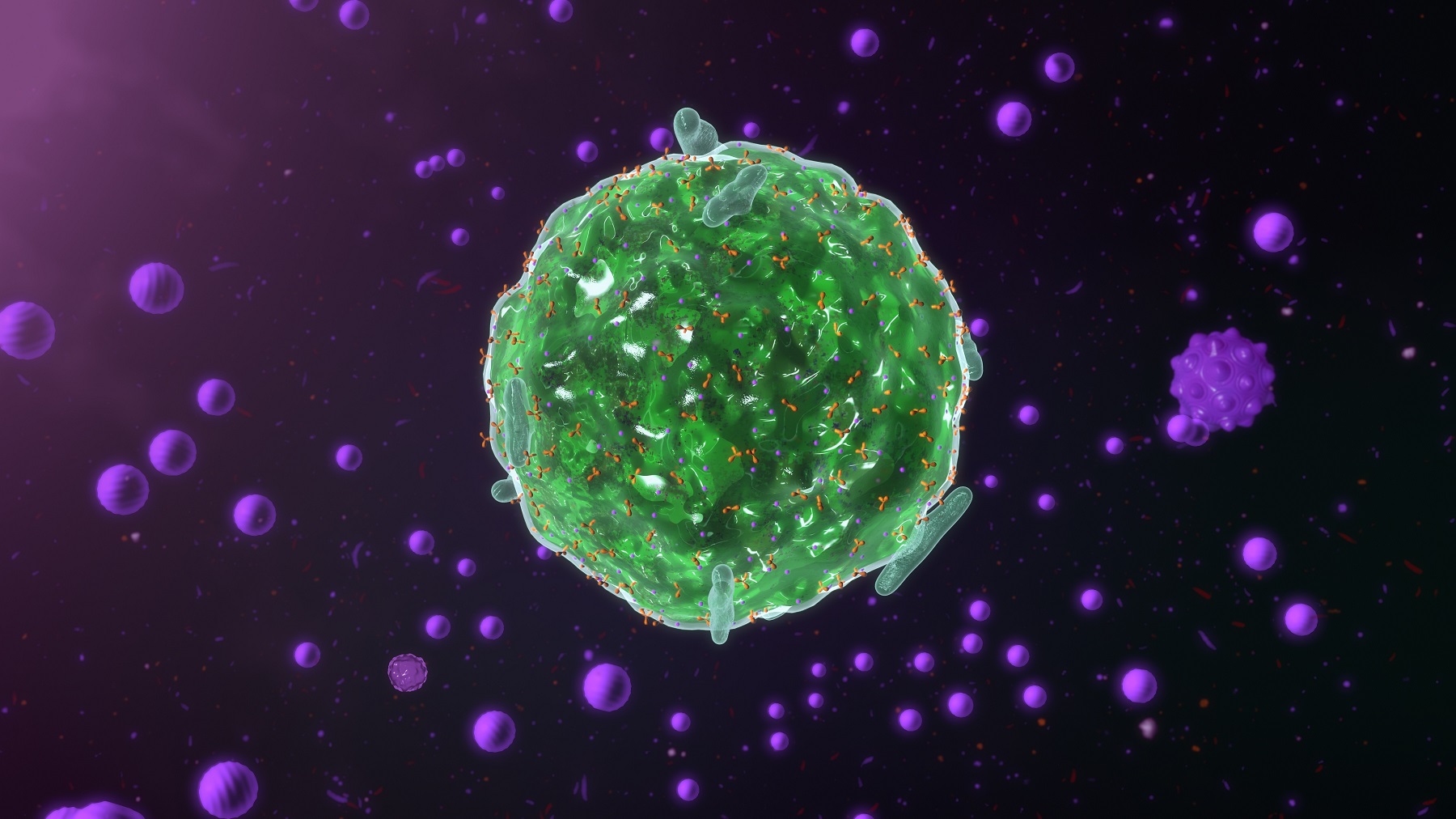
When most people have an allergic reaction, they can go to their medicine cabinet, take an antihistamine like BenadrylⓇ or ClaritinⓇ and they’ll get relief from their symptoms.
But have you ever experienced an allergic reaction where over the counter medications didn’t help – or even made your symptoms worse?
Maybe you’ve visited doctors and specialists with several other symptoms besides your allergies, but they can’t seem to pinpoint what’s wrong.
If that sounds familiar, you could have mast cell activation syndrome (MCAS). And if this is the first time you’re hearing of MCAS, you’re not alone.
Doctors and researchers have just started to recognize MCAS in the last decade. Also, many around the world may have MCAS but have never received a proper diagnosis.
I know it’s frustrating to not know what’s going on in your body – that’s why I’m dedicated to providing you the education you need. So, keep reading to see if you may have MCAS.
What Is Mast Cell Activation Syndrome (MCAS)?
Have you ever read headlines such as “‘Bubble girl’ is allergic to life” or “Minnesota woman allergic to husband”? These individuals were diagnosed with mast cell activation syndrome (MCAS). But what is it?
First, let’s define where MCAS came from- mast cell activation disease (or disorder – MCAD). Expert on mast cells Dr. Lawrence Afrin uses the analogy of an iceberg. Think of MCAD like the whole iceberg. You’ll see part of the iceberg above the waterline, and the rest of the iceberg you can’t see unless you’re underwater.
The tip of the iceberg is mastocytosis. Mastocytosis is a type of mast cell disease; it’s a rare genetic disorder where you’re born with too many mast cells.
Now let’s make our way down the rest of the iceberg until reaching the waterline. The rest of the mast cell diseases above the waterline are named conditions of MCAD. Many of these patients experience chronic illnesses with general themes of inflammation, allergies, and/or abnormal growth in tissues.
So what about below the waterline?
Those MCAD are termed MCAS – mast cell activation syndrome. MCAS is different from mastocytosis because with MCAS, you have an appropriate number of mast cells. The mast cells are just overactive – they’re activated when they’re not supposed to be. You may be diagnosed with MCAS if your symptoms or findings from testing don’t fit with other forms of MCAD.
The rest of this article will explore MCAS in detail. In order to fully understand what MCAS is, you first need to understand what mast cells are.
What Are Mast Cells?
Mast cells are specific types of white blood cells of your immune system that are found in mucosal and epithelial tissues throughout your body – examples include your skin, gut, and lungs. They create barriers between you and the outside environment. Mast cells are your body’s first line of defense against foreign intruders like viruses, pathogens, allergens, and bacteria.
When you come in contact with a foreign intruder, your mast cells release chemicals that send messages throughout your body. These messages tell your body how to react. There are many different types of chemicals that mast cells release, but two of the most common ones are serotonin and histamine.
Serotonin is a neurotransmitter that regulates your mood and behavior, aids in digestion and sleep, and plays a part in addiction and motivation.
Histamine is a neurotransmitter that regulates processes such as gastric acid secretion, inflammation, and vasodilation regulation. You’ve probably heard of histamine when it comes to allergic reactions because histamine is released when you have an allergic reaction.
How Are Histamine Intolerance and MCAS Related?
Your mast cells can release more than 200 different types of chemical messengers which may or may not include histamine. So, if you have MCAS, it’s not guaranteed that the overactivation of your mast cells involves histamine – because it may only involve other chemicals. So not everyone with histamine intolerance has MCAS, and not everyone with MCAS has histamine intolerance. However, histamine is a common chemical so many with MCAS also have histamine intolerance. Confused yet?
You get histamine intolerance when your mast cells are releasing too much histamine. In the most severe cases this can lead to anaphylaxis which is dangerous and can lead to death, however, many other less severe symptoms can occur. Either way it’s important to recognize the signs and symptoms you’re experiencing and to get treatment.
What Are the Signs and Symptoms of MCAS?
Mast cells are in various tissues, but they predominantly reside in perivascular sites and environmental interfaces (places your body interacts with the outside world). Therefore, most of the MCAS signs and symptoms someone experiences involve these areas. The MCAS signs and symptoms differ from person to person, but some common signs and symptoms include:
Skin Sensitivity
- Your skin may be sensitive to personal care products such as synthetic shampoos, conditioners, lotions, deodorants, skincare products, and makeup.
- You may be sensitive to bandaids, medical tape, and other adhesives.
- Your skin may redden quickly and easily.
- You may have an overreaction to bug bites and your skin may get itchy very easily.
- You may experience a rash from clothing due to specific fibers, materials, detergents, or clothing tags.
- Your skin may recognize if there are changes to temperature or pressure outside. You may experience increased allergies or rashes from these changes.
Digestive System
- You may experience an itchy mouth or throat when you eat specific foods.
- You may experience your throat closing when you eat something.
- Your stomach may hurt when you eat specific spices or seasonings, drink specific drinks, or consume artificial dyes or ingredients.
- You may experience nausea, vomiting, acid reflux, abdominal pain, cramping, diarrhea, and/or constipation.
Reproductive and Urinary System
- Many females with MCAS experience irregular, heavy, and painful periods.
- You may experience frequent and/or painful urination.
- Your body may experience inflammatory problems.
Upper and Lower Respiratory Tract
- Similar to an allergic reaction, you may experience nasal congestion, itchy/watery eyes, or even shortness of breath, wheezing, or asthma. Keep in mind these symptoms may be exacerbated by a variety of products like artificial fragrances from air fresheners and perfumes, smoke, and/or car exhaust, not just foods and environmental allergens.
Neurological System
- Going through an undiagnosed disorder for many years – even decades – can be stressful in and of itself. However, there are other neurological symptoms you can experience with MCAS.
- You may experience panic attacks, anxiety, depression, insomnia, brain fog, headaches, and/or migraines.
Immune System
- You may experience increased infections or susceptibility to infection.
- MCAS may lead to increased difficulty in healing infections and wounds and an increased risk for certain malignancies.
- Without a proper immune system, you may have an increased risk of developing autoimmune conditions.
Now, this isn’t a complete list of MCAS symptoms. Many people with MCAS can experience a variety of symptoms, and sometimes patients can present symptoms so unrelated to each other that it’s difficult to diagnose for MCAS. It’s important that you work with your medical providers to determine if you have MCAS. So let’s explore how to diagnose it next.
How Can You Get Tested For MCAS?
Before you treat your MCAS, it’s important and beneficial to get tested and receive a diagnosis for it. When it comes to diagnosing mastocytosis, many doctors will measure certain levels with blood and/or urine and/or perform a bone marrow biopsy. However, these tests aren’t always very helpful for diagnosing MCAS.
In order to test for MCAS, it’s helpful to measure 10 markers specific to the mast cell. These markers include:
- Tryptase and chromogranin A in serum – You’ll need to determine your health history before testing because abnormalities to chromogranin A may be due to issues such as heart or renal failure, use of proton pump inhibitor, or neuroendocrine cancer.
- Prostaglandin D2, histamine, and heparin in plasma
- Prostaglandin D2, 2,3-Dinor-11beta-prostaglandin F2 alpha, Histamine, N-methylhistamine, and leukotriene E4 in urine
Testing for these markers can be expensive and there may not be a lab that tests for all 10 of these markers. Discuss options with your medical doctor to see which tests are needed for you.
How Do You Treat MCAS?
Unfortunately, there isn’t a cure for MCAS. There also isn’t a one-size-fits-all when it comes to treating MCAS. Many individuals with MCAS may be experiencing other conditions such as polycystic ovarian syndrome (PCOS), chronic infections like lyme, postural orthostatic tachycardia syndrome (POTS), or autoimmune disease for example. This is why it’s crucial to work with your doctor to minimize complications in your treatment plan.
I’ve found that when it comes to treating MCAS in my patients, the first step is to identify triggers and work with my patients to avoid the triggers. The second step is to have the patient take certain supplements and/or medications that have antihistamine and/or mast cell stabilization effects to improve their results. Lastly, I work with my patients to look for root causes and contributors to their symptoms, like a vitamin D deficiency, food allergies, or chronic infection for example.
Here are some tips and treatments that I’ve used with my MCAS patients at our functional medicine clinic:
- Eat a low histamine diet
Histamine can be found in certain foods. Some foods to avoid if you have MCAS include:
- Fermented vegetables like kimchi, sauerkraut, and pickles
- Fermented dairy products like sour cream, buttermilk, kefir, aged cheese, and yogurt
- Kombucha
- Wine, beer, and alcoholic beverages
- Tomatoes
- Eggplant
- Spinach
- Vinegar
- Processed foods
- Avoid leftovers
How you prepare your food is important too. Frying and grilling foods show an increase in histamine levels while boiling food decreases or doesn’t influence histamine levels.
- Avoid known food and environmental allergens
It may be helpful to take allergy tests. Speak with your doctor to determine what foods or environmental allergens are increasing the number of histamines that you’re exposed to.
In addition to the food allergens mentioned above, other food allergens include dairy, vinegar, and preservatives.
Environmental allergens include mold, heavy metals, and airborne chemicals.
- Consider taking nutritional supplements
Some nutrition supplements I common;y recommend are:
- Vitamin C: Vitamin C naturally lowers histamine by helping the body produce diamine oxidase (DAO), an enzyme that degrades histamine.
- N-Acetyl Cysteine (NAC): Just like vitamin C, NAC can break down histamine. It also supports liver health.
- Quercetin: Quercetin can help to stabilize mast cells and reduce symptoms of their overactivation. It can inhibit the release of histamine and other MCAS mediators.
- Stinging nettles: Stinging nettles are plants that can be used to make teas and soups. They contain a high amount of quercetin.
- Bromelain: Bromelain is a group of enzymes found in the pineapple plant. It’s a natural source of antihistamines that compete with histamine to bind to histamine receptors on cells. This can help to reduce MCAS symptoms.
- Butyrate: Butyrate can benefit body systems such as the gut in many ways. It can support the immune system and reduce the symptoms that come from mast cells.
These are just a few nutritional supplements that may work for you. Talk with your doctor to determine which supplements would work best for your MCAS regime and treatment plan.
- Consider taking medications
Some over-the-counter and prescription medications can also help reduce your MCAS symptoms. Some medications to ask your doctor about include:
- H1 blockers: Claritin® (loratadine), Zyrtec® (cetirizine), Allegra® (fexofenadine), and Xyzal® (levocetirizine). Because MCAS may cause lethargy, taking a non-sedating H1 blocker would be helpful.
- H2 blockers: Pepcid® (famotidine), Zantac 360°™(ranitidine), Axid (nizatidine), and Tagamet (cimetidine)
- Mast cell stabilizers: Cromolyn and Ketotifen
- Leukotriene inhibitor: Singulair
- Low dose naltrexone
If you’re on any other medications, be sure to speak with your doctor to ensure that your prescription medications won’t interfere with each other. It is not always appropriate for all patients to take all classes of the above medications–this is highly individualized.
If you’ve liked to keep up with the latest in MCAS research, I highly recommend reading publications and resources by Dr. Lawrence B. Afrin and Dr. Leonard B. Weinstock. One of their research studies confirmed that mast cells are activated SARS-CoV-2 and may play a pivotal role in COVID-19 long haulers and the long-term effects they are experiencing from the virus. It will be interesting to learn more about this from future studies.
Let’s Control Your MCAS
Choosing a health team that works together is key to getting to the root cause of your allergic reactions! If you do have MCAS, choosing a functional medicine doctor that understands this disease will help tremendously. They can help you co-create a treatment plan that works for your lifestyle and will provide you long-term results.
If you’re in the Paradise Valley/Scottsdale/Phoenix area, my team is currently accepting new patients at Arizona Wellness Medicine. To schedule an appointment or ask a question please reach out through our contact form.
Did you learn something about MCAS? Share with me in the comment section below!
Here’s to your health and wellbeing,
Dr. Emily Parke
Share:
Dr. Emily Parke
Related Posts

What Is Sleep Apnea? Symptoms, Risks, and Treatment Options
Sleep apnea occurs when breathing repeatedly stops and starts throughout the night. Learn the symptoms, risks, and sleep apnea treatment options.

Estrogen Metabolism: How It Works, Why It Matters, and Supplements for Healthy Estrogen Metabolism
Estrogen metabolism is vital to estrogen regulation. Learn how it works and how the DUTCH test can provide insight into hormonal imbalance.

The Paleo Diet Versus the Autoimmune Paleo Diet: Differences and Benefits
Learn the difference between the paleo and the autoimmune paleo diet, including food lists, what foods to avoid, and all the health benefits!
A Complete View of Multiple Sclerosis: Symptoms, Diagnosis, and Functional Medicine Treatment Options
Get a complete view of multiple sclerosis, including common symptoms and treatment options, including nutrition and supplementation.
